In this post
Lorem ipsum dolor sit amet
Lorem ipsum dolor sit amet
Over the last three years, GLP-1s have moved from niche treatment to mainstream benefits strategy. They work, employees want access, and employers need a way to offer support without destabilizing healthcare budgets.
GLP-1 Demand Is Surging Fast
GLP-1 medications are highly effective for weight health and chronic conditions, but they remain one of the most complex coverage decisions employers face. These drugs are also a leading contributor to a projected 9% increase in healthcare costs in 2026.
Employer coverage patterns show just how unsettled the market still is. According to the International Foundation of Employee Benefit Plans, as of 2025:
- 55% of employers cover GLP-1 medications only for diabetes through their health plans, down from 57%in 2024
- 36% cover GLP-1 medications for both diabetes and weight loss through their health plans, up from 34%in 2024
Other sources report a much higher GLP-1 coverage for weight loss, between 49% and 57% among employers. Eligibility criteria are broad. Individuals with a body mass index (BMI) over 30 are eligible for GLP-1s, as are individuals with a lower BMI and a qualifying chronic condition.
At the same time, pricing varies depending on how access is structured. Across both Wegovy and Zepbound—the only two GLP-1s that are FDA-approved for weight loss—direct-to-consumer, or cash-pay pricing is 40-60% lower than what employers pay through traditional health plan pharmacy benefits.
The implication is clear. As Pharmacy Benefit Management (PBM) costs face continued policy pressure, it’s unsurprising that a growing majority of employers are exploring cash-pay access models, like pharmacies and weight loss programs, to control spend and improve predictability. Covering GLP-1s through the core medical plan often leads to higher premiums, reduced flexibility, and long-term cost risk. As a result, many organizations seek alternatives that provide access without permanently embedding GLP-1 costs into the medical plan.
Specialty HRAs Explained Simply
A Health Reimbursement Account (HRA) is an employer-funded account that reimburses employees for eligible healthcare expenses. Employers define the budget and eligibility rules. Employees choose the care that fits their needs.
Specialty HRAs narrow the focus to specific healthcare needs rather than covering everything. Common use cases include mental health, fertility, medical travel, gender-affirming care, and weight health. With more than 200 IRS 213(d) categories available, Specialty HRAs allow benefits leaders to design programs that reflect real employee demand.
This structure delivers cost control without sacrificing care.
Where Specialty HRAs Get Tricky
The value of a Specialty HRA depends heavily on the platform administering it. Not every vendor can support the level of customization employers need.
When exploring HRA solutions, benefits leaders should ask:
- Can we customize the HRA so employees clearly understand their eligible expenses?
- Can we apply exclusions, such as blocking purchases from specific vendors or stores?
- Can we restrict purchases to specific medications?
- Is there a true card-first experience using a VISA card at point of sale?
- Are reimbursements fast, or must employees wait weeks to be paid back?
- What type of reporting is available to capture utilization and other metrics?
Without modern infrastructure, Specialty HRAs can add friction instead of flexibility.
Why Benepass Is Building Weight Health HRAs
Today, Benepass supports several specialty HRAs including a Weight Health HRA for GLP-1 medications.
This model separates GLP-1 spending from the medical plan while giving employers clear budgets and employees a seamless experience.
.webp)
How Weight Health HRAs Work in Real Life
Employers working with Benepass define eligibility criteria, set fixed budgets, and customize coverage rules for their GLP-1 and weight health programs. Here’s how it could work:
James, 36, Company A
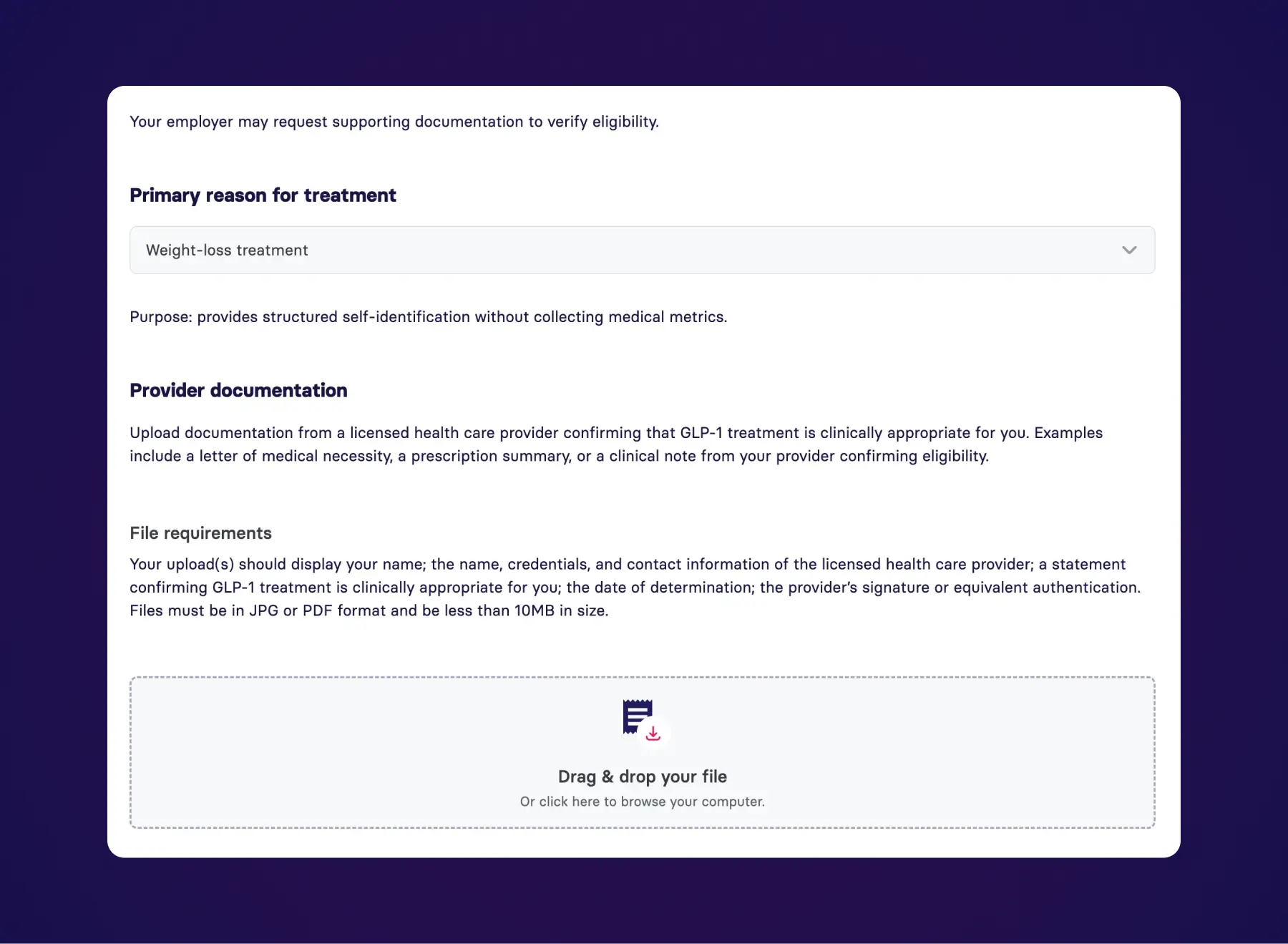
James has a high BMI and has seen a growing number of GLP-1 ads online. His employer offers a Weight Health HRA for GLP-1 medications. Inside the app, James can clearly see which medications and expenses are covered. After submitting a letter from his doctor confirming his BMI, his HRA funds unlock. Crucially, his Benepass card only works for specific FDA-approved medications and as defined by his employer, giving him confidence and protection.
Why Employers Are Zeroing In On GLP-1s
The numbers tell the story:
- 40% of US adults are living with obesity, with projections closer to 50% by 2030
- Employers spend $6,472 more per year on employees with obesity than on healthy-weight employees across medical, productivity, disability, and workers’ comp
- Individuals who use GLP-1s can lose between 2.5% and 20% of their initial body weight when taking the medication as instructed
Employers want to support prevention, not wait until employees are sicker to qualify for care. Specialty HRAs provide access without surrendering cost control.
Regain Control Of Weight Health Spend
GLP-1s are not a passing trend. Employers need a way to respond to growing demand without destabilizing their healthcare budget. Specialty HRAs provide a flexible, preventive approach by separating weight health from the core medical plan and setting clear contribution limits.
Alongside HRAs, Benepass also supports pre-tax weight health spending through HSAs and FSAs with clear education that helps employees use their benefits effectively. For global teams, Benepass advises on compliant weight health program design and administration across regions, helping employers apply a consistent strategy without losing local control.
Ready for a weight health program that moves in step with employee needs, without the fear of uncontrollable costs? Book a demo to learn how Benepass can support you.


